Having a ruptured or herniated disc, also referred to as a “slipped” disc, can be very painful, but so are many initial back injuries. In fact, most active people who play sports or exercise are all too familiar with back pain that may mimic symptoms of a herniated disc, but understanding how a rupture can affect other nerves is the key in knowing how to differentiate this from pain caused by other conditions.
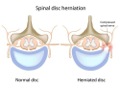 As most readers know, the spine consists of small bones called vertebrae that are stacked one on top of another in a configuration that supports the weight of your body; the spinal column protects your spinal cord and connected nerves. Between each set of bones is a disc that acts as a shock absorber. Each disc is composed of two components: An outer shell of strong material; and an inner core of a jelly-like substance called the nucleus pulposus, which the vertebral disc to withstand forces of compression and torsion.
As most readers know, the spine consists of small bones called vertebrae that are stacked one on top of another in a configuration that supports the weight of your body; the spinal column protects your spinal cord and connected nerves. Between each set of bones is a disc that acts as a shock absorber. Each disc is composed of two components: An outer shell of strong material; and an inner core of a jelly-like substance called the nucleus pulposus, which the vertebral disc to withstand forces of compression and torsion.
A rupture or herniation occurs when a disc ages or is damaged by trauma and a small penetration develops in its protective outer shell, allowing small amounts of the jelly-like nucleus pulposus to escape. For a quick visualization, imagine what happens when you squeeze a jelly-filled donut and see the jelly squirt out the hole of its side.
According to the American Academy of Orthopaedic Surgeons, a herniated disc can affect a nerve’s roots in one of two ways: The first and most obvious mechanism is through sheer pressure. As the disc ruptures, forcing the jelly-like nucleus pulposus into your spinal canal, the viscous material can pin your nerve roots against the borders of your spinal canal, causing physical trauma to the nerve roots. The second way a herniation affects a nerve root is by the very nature of the chemical make-up of the nucleus pulposus. The substance is very irritating to nerves and causes a significant inflammatory response when it contacts a nerve root. This explains why even a minimal disc herniation, which may exert insignificant physical pressure on nerve roots, can still be extremely painful.
Symptoms will vary depending on the location of the ruptured disc. Literature on disc herniation offered by the American Medical Association outlines several scenarios for ruptures in different areas of the spinal column: A ruptured disc in your neck may cause pain around your neck, shoulder blade or running down your arm. A disc rupture in your lower back can cause low back pain and sciatica (buttock, and leg pain that shoots down either leg). Some patients describe it as electricity or feeling like their leg is on fire. Other symptoms include pins and needles, or numbness and tingling.
 More severe disc ruptures can result in weakness in the muscles in your arms or legs as a result of pressure on the nerves controlling those muscles. In extreme cases, they can cause loss of control over your bowel and bladder. Your pain will tend to increase with coughing or sneezing and with sitting down. In order to make the diagnosis, your doctor will perform a history and physical exam to see if your symptoms are consistent with a ruptured disc. If appropriate, a MRI of your neck or back may show the exact location and size of the herniation.
More severe disc ruptures can result in weakness in the muscles in your arms or legs as a result of pressure on the nerves controlling those muscles. In extreme cases, they can cause loss of control over your bowel and bladder. Your pain will tend to increase with coughing or sneezing and with sitting down. In order to make the diagnosis, your doctor will perform a history and physical exam to see if your symptoms are consistent with a ruptured disc. If appropriate, a MRI of your neck or back may show the exact location and size of the herniation.
With the goal of relieving discomfort and preventing any permanent injury to your nerves, treatments range from medications and physical therapy to epidural steroid injections or surgery. Depending on the location and size of the disc, surgical intervention may be necessary.
The key is getting a proper diagnosis early, so your doctor can determine which treatment will prevent your condition from worsening. As with most injuries, the sooner you take care of a herniated disc, the more likely you’ll be able to recover without lasting pain or damage.

